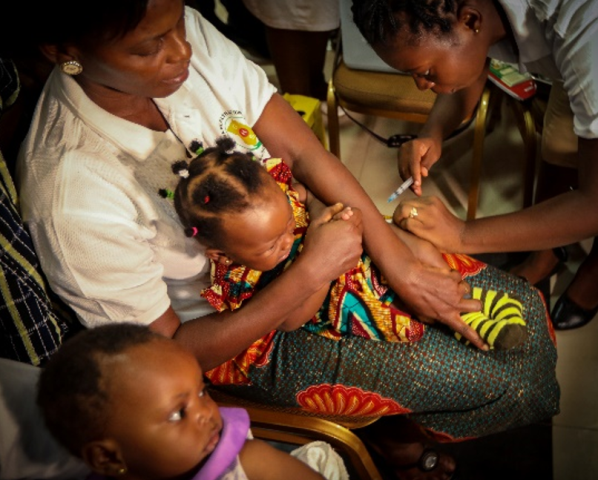
 WHO photo: Susana and Abigail are first to be vaccinated with the malaria vaccine in Ghana pilot. [Credit: WHO/Fanjan Combrink]
WHO photo: Susana and Abigail are first to be vaccinated with the malaria vaccine in Ghana pilot. [Credit: WHO/Fanjan Combrink]
A child in Africa dies every minute from malaria and more than 3 billion people are at risk from the disease. Now a vaccine to prevent one of the developing world’s biggest killers may finally be within reach. After more than three decades of research and almost $1bn, a pilot programme to test the vaccine has begun in Malawi, Kenya and Ghana.
With four species of the Plasmodium parasite needing humans as a host, malaria is as old as civilisation; mentioned in Mesopotamian clay tablets and India’s Vedic writings, it was spread by humans wherever we went. In the 20th century up to 300 million people died from malaria. While insecticides and draining swamps helped eradicate malaria in the southern US by 1951, the search for a prophylactic began in 1955 when the World Health Organization (WHO) boldly proposed eradication. This was already being hindered by resistance to frontline antimalarial drugs such as chloroquine and mefloquine. Science described how insecticides also became ineffective; DDT became useless in many regions by the 1960s and resistance to pyrethroid, first detected in Ivory Coast in 1993, has now spread across Africa.
So the $52m pilot programme for the RTS,S vaccine, which reduces cases in children by up to 40%, is being hailed as a significant step forward. Even though RTS-S does not protect most children, anyone vaccinated who develops malaria is likely to have less severe cases, trials found. Over the next four years a million babies in Ghana, Malawi and Kenya could be vaccinated with four doses of RTS,S. ‘This is really something we are considering in public health as a dream coming true,’ said Dr Richard Mihigo, of the WHO.
However, there are concerns over the practicality of dosing – once a month for three months and again at 18 months – and the relatively high cost, at $5 each. Health experts cautioned that the vaccine would only ever be one of many weapons deployed against malaria, alongside bed nets, insecticides and prompt testing and treatment.
Free impregnated bednets have been highly effective in controlling malaria in recent decades, with the number of people able to use them rising from 2% to 49% globally in the decade to 2013. But another problem arose there as researchers realised how many were used as fishing nets, endangering humans and fish stocks. The use of bed nets as wedding veils and dresses has declined in east Africa at least after an information campaign was launched. And other innovations may help the war on malaria, such as the rollout of drones to deliver vaccines to 2,000 remote health centres in Ghana following its successful use in Rwanda.
But many researchers wonder whether the pilot programme itself is the best way to spend such large sums, Amy Maxmen noted in Nature. Another promising line of research is in genetically modifying mosquitoes so they pass on a lethal protein to their offspring. They are now being used in Brazil against the Aedes aegypti mosquito, which spreads dengue and Zika. However, the 100 or so variants of the Anopheles genus that transmit malaria present a more intractable problem. The fight against one of humans’ oldest enemies is far from over.



